Chapter 2: The long road home

Eric Waksmunski holds both twins, Shane, left and Wyatt, at home for the first time after Wyatt was released from the hospital. (All photos by Bob Ford/Times News)
Anticipating the usual complications faced by premature babies, the couple also had to face the unexpected when both Shane and Wyatt were diagnosed with Down syndrome. According to the National Down syndrome Cytogenetic
Before they could appreciate how rare their situation was, or how much their lives were about to change, the couple had to deal with the reality of their situation. Their babies were seriously ill.
Over the next few months they would face multiple surgeries and numerous infections. They would stop breathing or lose consciousness, and on at least one occasion, required CPR. It seemed for awhile that every day they faced a new challenge and a new danger, but eventually, after four months of hospitalization, with just a brief trip home for Shane, both babies would be well enough to leave the hospital.
Chapter Two of Shane and Wyatt’s story is about that long, hard journey home.
By KAREN CIMMS
kcimms@tnonline.com When Mary Anne Christo gave birth in March, she and husband Eric Waksmunski were prepared for twins and for an early delivery, but the Mahoning Township couple was devastated to learn both boys had Down syndrome.
Shane and Wyatt faced the usual complications of babies born 10 weeks early. They needed
The babies also had feeding issues. Being premature, they didn’t have a sufficient suck reflex to bottle feed. Both were given nasogastric feeding tubes that went through the nose and into the stomach.
Shane weighed 3.5 pounds at birth, while Wyatt was 3.4 pounds. As most babies do, they lost weight after birth, each dropping to under 3 pounds.
While their early birth and Down syndrome diagnosis were serious, neither was critical. There was even talk of sending them home in a few weeks.
“It was our emotions that were critical,” Waksmunski recalls.
“Yes,” agrees Christo, “it was a bad time.”
Although Waksmunski and Christo, who are originally from South River, N.J., accept that their lives have changed, it was difficult in the beginning.
“The grief part of it took awhile to get over,” says Waksmunski. “But yet, that same day, March 6, that Saturday night, I was already on the Internet researching Down syndrome and already was thinking that we have to do something. I went into that mode instantly, but yet, I was still bawling my eyes out too.”
Christo remembers that night at St. Luke’s Hospital in Bethlehem well.
“It’s a good example of how men and women deal with grief and situations differently,” she recalls. “Because really, he was a rock to me, but he was still saddened and devastated and had all those feelings of loss, but he was able to quickly turn it and just say, ‘Well, if this is what it’s going to be, then this is how we have to deal with it.’”
As the weeks passed, Christo and Waksmunski dealt with their emotions and prepared to welcome the twins home. Waksmunski returned to his job as a regional loss prevention manager for Urban Outfitters, while Christo, who left her job as a registered nurse at Blue Mountain Health System months earlier due to complications with her pregnancy, cared for their son, Jesse, who was almost 3. They took numerous trips to Bethlehem, waiting for the day the doctors would let them bring their babies home.
By mid-April, it looked like that day was just around the corner. Wyatt was up to 5.13 pounds and Shane weighed 5.6 pounds. Wyatt was scheduled to go home April 30. Shane wasn’t to be too far behind him.
But days later, they learned Wyatt would not be going home, and there was discussion that Shane might need surgery.
The roller coaster ride was just beginning.
In early May, there was talk that Shane would be coming home. Wyatt was diagnosed with aspiration pneumonia (caused by breathing foreign materials into the lungs, in this case — formula), and would need to remain in the hospital awhile longer. Within days, Shane began to have a high number of apnea and bradycardia incidents. Doctors began to link the events to feeding issues, and expressed concerns about the babies aspirating. Discussion of a homecoming for either baby was put on hold.

Jesse sits on the couch with his mother as she holds Shane shortly after he came home from St. Luke's Hospital. At the time Shane was still getting his nutrients from a nasogastric feeding tube.
The apnea and bradycardia incidents began to increase, with Shane having 14 incidents in just one day. The doctors were concerned both babies had reflux issues, which meant the food they were eating was leaking back into the esophagus. Both boys were being fed during the night via feeding tubes. During the day, they were bottle fed small amounts of formula.
On Mother’s Day, May 9 — the twins’ original due date — there was still no more talk of when they would be going home. As the apnea and bradycardia issues continued to increase, bottle feeding was stopped and both boys remained on a continuous tube feed.
By the middle of May, medical personnel again discussed sending Shane home. One day it was on, the next day it was off.
Finally, almost 11 weeks after he was born, Shane went home, while Wyatt remained at St. Luke’s in the Neonatal Intensive Care Unit.
Home, but not for long
The Waksmunski’s dining room was turned into a nursery, with matching cribs and a changing table. The playful jungle-themed bedding and mobiles stood in stark contrast to a host of medical equipment — from oxygen to heart monitors, as well as overnight nursing care — that welcomed Shane home.
Shane’s first few days at home were uneventful, but that would not last. As his food intake increased, so did the number of reflux incidents.
On the evening of May 30, Shane’s heart monitor went off 10 times. The next day he was rushed to the emergency room.
Doctors at St. Luke’s suspected an infection and recommended he be transferred to a children’s hospital. The decision was made to take him to Janet Weis Children’s Hospital in Danville.
At Janet Weis, doctors discovered a growth near Shane’s testicles. Surgery the following day was deemed to be a success, but the next morning, as they prepared to take him home, Shane went unresponsive. Christo worked on reviving him while Waksmunski ran for help.
Shane had experienced severe reflux, which caused a vasovagal (or fainting) episode.
“I never knew, and I still don’t understand how reflux can trigger so many things,” says Waksmunski. “It can stop your heart; can stop you from breathing; it can put you unconscious, and I never knew all that.”
The Waksmunskis believe that while the babies were in the hospital, the amount of food they received was small enough to keep them from refluxing. When Shane came home and his food intake increased, even a little, he began to reflux more.
After Shane’s vasovagal episode, the doctors ran more tests.
“They said ‘this kid’s in bad shape,’” recalls Waksmunski.
The couple now had two very sick babies, in two different hospitals, over two hours away from each other.
Wyatt takes a ride
Doctors at Janet Weis consulted with doctors at St. Luke’s and determined Wyatt was having the same problems as Shane. It was recommended he be transferred to Janet Weis.
Before he had his first car ride or slept in his own crib, Wyatt took his first helicopter ride, flying 120 miles from Bethlehem to Danville.
In the meantime, surgery was again discussed for Shane. Doctors recommended a procedure called fundoplication, which would create a flap at the bottom of the esophagus, and prevent food in the stomach from refluxing into the esophagus. They also wanted to insert a gastrostomy feeding tube (G-tube), which would be placed through his abdomen into his stomach. Wyatt would likely face the same procedure.
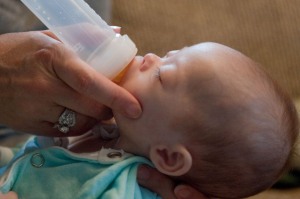
Mary Anne Christo uses her fingers to support Shane's mouth and initiate a sucking motion. Both boys had difficulties with their sucking reflex after they were born, which is common with premature babies.
In addition to dozens of public comments on Facebook, he received nearly 100 e-mails from parents, which included telephone numbers so he could call them back to discuss their experiences. That input, coupled with research and an understanding of the needs of his children, helped him also agree to the surgery.
When Wyatt experienced an incident similar to Shane’s, it was decided that he too would have the surgery.
On June 11, Wyatt was wheeled into surgery first, followed by Shane. Afterward the babies were moved to separate rooms on the pediatric floor.
Both surgeries went well, but by late evening it was clear Wyatt was in crisis.
“Wyatt didn’t seem to be doing well after the surgery,” recalls Christo. “It was apparent that he was really struggling — struggling to breathe, struggling to survive.”
She held an oxygen mask to Wyatt’s face and over the course of the evening, his heart rate and oxygen levels continued to drop.
Waksmunski decided to find a nurse and request a nasal cannula, which would secure the oxygen tube to Wyatt’s nose. Almost the moment Waksmunski left the room, Wyatt coded.
“All of a sudden, he literally crashed, and babies can crash very quickly,” explains Christo. “Eric probably got outside the door, and I thought that I (whispered) ‘Rick,’ but instead, I had yelled, and he had heard me. I just started CPR immediately because I wasn’t going to take time to start yelling. I just put the baby down on the bed and started CPR.”
Waksmunski came back into the room and hit the panic button.
Christo continued CPR until the hospital staff took over.
“He was death blue,” says Christo. “I know what a dead baby looks like, and when I put him on the bed to do CPR, I thought he was dead. I truly did.”
Although the stress of the past couple months could have put Christo over the edge, she admits that remaining calm in the face of a crisis is her strongest trait.
“In times of stress, if someone is hurt or sick, I am able to remain calm and not lose focus. That quality saved my son’s life,” says Christo.
“When it comes to health, and I think that’s because I was raised by a mother who was always ill, I’m always calm,” Christo continued. “I’m always able to hold my head, and that’s how I was. When that happened, it just felt like my brain had split into 20 pieces. It was like ‘OK. Remain calm. OK. Start CPR.’ All these little things. I didn’t lose it until after I stepped away and they started working on him.”
“You became a mom again,” recalls Waksmunski.
More rough days ahead
It turned out that Wyatt, and apparently Shane as well, had a reaction to the morphine given to them after surgery, and it suppressed their breathing. They were both moved back into the pediatric intensive care unit.
“There were a number of times they needed advanced care to resuscitate after that,” says Waksmunski. “They were in real critical care for that time period.”
The next day, after a long stressful week, much of it spent at the hospital, the Waksmunskis checked in on their sons before heading home to see Jesse and to sleep in their own bed.
When the phone rang sometime after 8 p.m. that night, it was not good news. Wyatt was being rushed back into surgery. His incision had opened and his bowel was exposed, putting him at high risk for infection. The Waksmunskis set out on the two-hour drive back to the hospital.
During surgery, one of Wyatt’s lungs partially collapsed and he was placed on a ventilator.
Back at home the next night, the surgeon called about Shane. His incision was leaking and there was again concern about infection.
The next morning, they were advised that Wyatt’s condition had worsened and he was being moved into isolation in the PICU as it was suspected he had a virus or an infection. His lung hadn’t improved and he would remain in a drug-induced coma and on a ventilator. Later in the day, another call advised them that Shane may be heading back to surgery.
The following day, Wyatt was improving and plans were made to begin weaning him off the ventilator, but later in the day, he crashed again.
The stress was clearly getting to the Waksmunskis. Almost every day they were faced with life-and-death situations.
And it wasn’t getting any better.
The next evening, after leaving the hospital and heading home, they got a phone call just a mile from their home. Shane was being rushed into the operating room. They emptied their suitcases, filled them with clean clothes, and headed back to the hospital.
Shane came out of surgery around 2:45 a.m. He was put on a ventilator as his left lung wasn’t ventilating.
After a few days with no major incidents, medical personnel again discussed sending the boys home.
But again, things went awry.
On Father’s Day, just after midnight, the phone rang. Wyatt was running a fever and his white blood cell count was very high. After a spinal tap, doctors suspected meningitis or some other type of infection. There was even some concern about leukemia.
Shane was showing similar signs; no fever, but his white blood cell count was rising. The boys were put on antibiotics to fight the infection.
“They really went through a couple-week period where it was really life or death, because they weren’t reacting well,” recalls Waksmunski. “They were having infections. They kept going back into surgery and what had happened was they took a beating on their little bodies, and then that’s when they put them both on ventilators and put them in a drug-induced coma for a few days to rest them, because they said ‘We can’t keep doing this. They’re not going to survive.’”
Near the end of June and after almost four months of hospitalization and weeks of life and death moments, the twins began to have more good days than bad. They were still fighting infections and setbacks, but they were feeding and slowly growing stronger. It also appeared the fundoplication surgery was working.
“They’re feeding, and they’re feeding by bottle,” says Waksmunski, “and they are not having the apnea and heart rate issues. They seem to be doing better.”
Although the twins were still in the seven-pound range a couple weeks after surgery, their ability to keep food down was enabling them to start gaining weight — something they both desperately needed.
A long time coming
After months in the hospital, thousands of miles in the car, tens of thousands of dollars in gas, food and hotel expenses, and over $2 million in medical expenses, the time finally arrived.
Shane and Wyatt were coming home!

The Waksmunski's SUV heads up the driveway on July 5 with Wyatt inside. Wyatt spent the first four months of his life in a hospital.
“TODAY!!! We are heading to the hospital soon to get Shane. HEY SHANE, Mama and Papa are coming to bring you home, again … for good! Wyatt, coming back Monday for you so pack your bags and get ready to start life at home. Four months is way too long to stay in the hospital. One day, we are going to Disneyland!!!!”
And true to those words, three days later, Wyatt came home.
Keep reading the TIMES NEWS for future stories on the Waksmunski family and their journey with Down syndrome. You can also log on to the TIMES NEWS website at www.tnonline.com for this and all of the stories in the series, “Down syndrome: A family’s journey.”
Feeding tubes and fundoplication
By AMY MILLER amiller@tnonline.comOver the last few months, Shane and Wyatt Waksmunski have experienced numerous treatments to help them take in essential food and nutrients; as well as be able to keep it down. Here is a list of procedures and devices that have been used to help the twins grow stronger.
Big brother Jesse checks out one of his new baby brothers after Shane came home from Janet Weis Children's Hospital.
Fundoplication surgery is used to help individuals with chronic gastroesophageal disease or GERD.
According to Dr. Ahmed Hasan, chief of gastroenterology at Blue Mountain Health System and a board certified gastroenterologist and internist, GERD occurs when the lower esophageal sphincter (LES) valve, located at the base of the esophagus, does not fully close, resulting in stomach acid and contents backing up into the esophagus, causing excessive heartburn, overall discomfort, and sometimes vomiting.
When GERD or acid reflux cannot be controlled by medications in children, fundoplication surgery may become an option.
Dr. Ronald Scorpio, director of pediatric surgery and surgeon-in-chief at Janet Weis Children’s Hospital, and the surgeon who treated Shane and Wyatt, explained that fundoplication is “an operation to create a valve at the bottom of the esophagus to prevent food from leaving the stomach and going back into the esophagus.”
The procedure, which takes a portion of the upper stomach and wraps it around the base of the esophagus, will usually restore the proper function of the LES without obstructing food intake.
Scorpio noted that excessive acid reflux and GERD in infants is typically more severe and could cause pneumonia or other complications.
There are benefits and risks to the surgery, Scorpio and Hasan both explained.
Benefits to having the fundoplication surgery include the improvement of digestion in the patient, no more reflux, and helps children get the nutrition they need.
Risks include trouble swallowing, not being able to vomit or belch, infections at the surgery site, anesthesia reactions, and the procedure not taking and becoming undone.
Scorpio said that the procedure is usually a long-term fix to a child’s reflux problem, but sometimes it fails. In children with health problems, a higher failure rate has been reported. If the procedure fails and symptoms return, the child is reevaluated to see how severe the reoccurrence of reflux is and if surgery is necessary or if it can be managed through medications.
Feeding tubes
There are four types of feeding tubes that the twins experienced: NG-tube, NJ-tube, G-tube and MIC-KEY button.
The NG- and NJ-tubes are both short-term feeding tubes that allowed the infants to receive the nutrition and medications they needed.
Both tubes are passed through the nasal passage. The NG-tube, or nasogastric-tube, ends in the child’s stomach. It is usually inserted to help the stomach drain or to give the child the food he needs to survive.
The NJ-tube, or nasojejunal-tube, goes one step farther. After being inserted into the nose, it travels through the stomach and into the small bowel or jejunum. The child is then given food and medications without worrying about reflux.
A G-tube, or gastrostomy-tube, is similar to the NG- and NJ-tubes, in that it provides a way for the child to receive necessary nutrition.
The G-tube is inserted directly into the stomach through the child’s belly wall. It is done through a procedure known as esophagogastroduodenoscopy or EGD. During the procedure the doctor cuts a small incision into the left side of the abdomen and inserts a flexible tube with a special tip or balloon into the opening.
Scorpio added that a child who has the fundoplication surgery usually has a G-tube.
The MIC-KEY button functions the same as the G-tube, except instead of a tube extending from the child’s body, a port or button is inserted into the incision and lies flat on the belly.
Scorpio said that when it is time to feed the child, a flexible tube is attached to the button and then functions like a G-tube.


No comments:
Post a Comment